Recovery is one of the most important and often most worrying parts of having surgery. Many patients focus on ....
- Please wait..
Doctify Team
Hyaluronic acid (HA) has become a skincare essential for anyone seeking smooth, hydrated, and radiant skin. Nevertheless, not all ....
Doctify Team
Many people experience fatigue, tiredness, weight gain, mood changes, or even anxiety and dismiss them as stress or lifestyle ....
Doctify Team
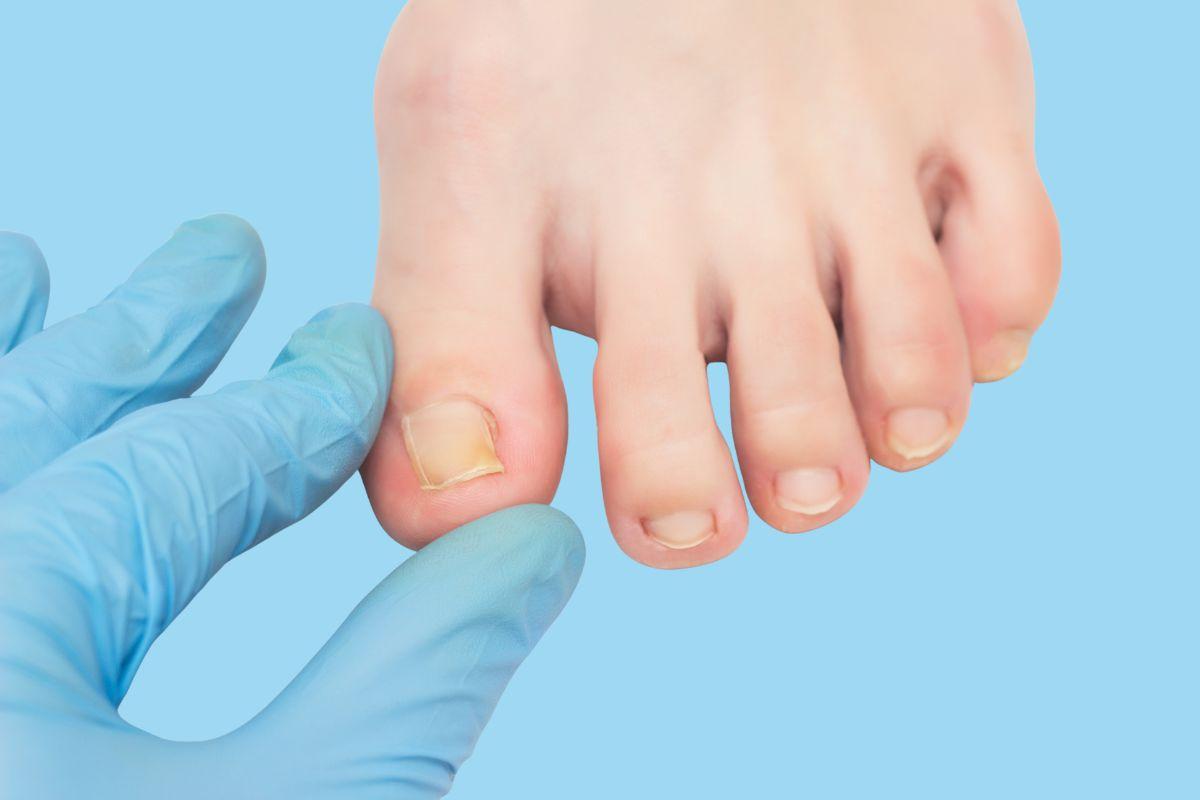
Nail psoriasis can be both frustrating and uncomfortable. It not only affects how your nails look but can also ....
Doctify Team
Losing a significant amount of weight is an incredible achievement that can transform both your health and your confidence. ....
Doctify Team
Acid reflux can disrupt daily life — from constant heartburn to sleep disturbance. While most cases respond well to ....
Doctify Team
Living with asthma can sometimes feel unpredictable, especially when symptoms flare up without warning. Breathlessness, wheezing, or chest tightness ....
Doctify Team
Nail fungus, also known as onychomycosis, can be a persistent and frustrating problem. Discoloured, thickened nails that resist every ....
Doctify Team
Dermal fillers have become one of the most popular cosmetic treatments for restoring facial volume and smoothing fine lines. ....